Polyethylene Glycol Treatment for Peripheral Nerve Repair in Preclinical Models
Davis B. Rippee1, Gabriella E. Glassman2, Sara C. Chaker3, Patrick E. Assi4, Jennifer Black, Alonda C. Pollins4, Jun Yao4, Wesley P. Thayer4,6*
1University of Mississippi School of Medicine, Jackson, MS, USA
2Florida State University College of Medicine, Tallahassee, FL, USA
3Vanderbilt University, Nashville, TN, USA
4Department of Plastic Surgery, Vanderbilt University Medical Center, Nashville, TN, USA
5Meharry Medical College, Nashville, TN, USA
6*Department of Orthopaedic Surgery, Vanderbilt University Medical Center, Nashville, TN, USA
Abstract
Introduction: Peripheral nerve injuries commonly result from trauma and can lead to devastating loss of sensory and motor function. A novel strategy to improve peripheral nerve regeneration is a chemical fusogen known as polyethylene glycol (PEG). Several animal studies have illustrated PEG’s potential to help prevent axon loss after peripheral nerve injury. However, the relative rate of success and potential complications of these studies have not been definitively shown in the literature. The purpose of this systematic review is to evaluate the literature regarding the success of PEG adjunct treatment after peripheral nerve injury in preclinical models.
Materials and Methods: The MEDLINE database was queried using the PubMed search engine with the following keywords and phrases: “polyethylene glycol” OR “PEG” AND “nerve” AND “fusion”. All resulting articles were screened by two reviewers. Animal type, nerve type, injury type, type(s) of analyses, and overall superiority of outcomes were assessed.
Results: One-hundred and seventy-nine articles were identified, and thirteen studies remained after the application of inclusion and exclusion criteria. Twelve of the thirteen studies utilized rats as the preclinical model, while one utilized a guinea pig. Superiority of peripheral nerve repair outcomes with adjunct PEG treatment compared to a control group was reported in eleven of thirteen studies.
Conclusions: The majority of studies reported positive outcomes when using PEG; this indicates that PEG treatment has the potential to enhance peripheral nerve regeneration after injury. However, the results of some of these studies indicated several uncertainties that need to be addressed in future studies. These preclinical models may help guide clinicians regarding the use of PEG treatment in peripheral nerve repair.
Introduction
Twenty million Americans suffer from peripheral nerve injuries each year; these injuries result in billions of dollars worth of healthcare expenses each year in the United States1. The vast majority of these injuries are due to trauma and they disproportionately affect those in careers that involve a high risk of traumatic injury. The most commonly affected demographic are males under the age of 40 and the most commonly damaged peripheral nerves include the ulnar, radial, and median nerves2.
Peripheral nerve injuries can have a devastating impact on a patient’s quality of life. Symptoms include sensory and motor deficits that can result in paralysis of the affected limb and/or intractable neuropathic pain. Time is of the essence when treating these injuries, as muscle atrophy will ensue if repair is delayed.
Although there have been significant advancements in surgical technique and technology with regards to peripheral nerve repair over the past several decades, regeneration and recovery after these injuries remains problematic. Few patients with peripheral nerve injuries of the median and ulnar nerve achieve satisfactory motor recovery, and even less experience satisfactory sensory recovery4.
Many clinicians believe the predominant factor for the poor outcomes following these injuries is a failure to reestablish membrane continuity in the nerve3. This theory has led clinicians to seek out a variety of therapeutic measures that promote axonal fusion, including polyethylene glycol (PEG). PEG is produced by the interaction of ethylene oxide with water or ethylene glycol5. When combined with a calcium-free solution PEG can promote the fusion of axon plasma membranes and prevent the axon loss that occurs in Wallerian degeneration following peripheral nerve injury.
Discontinuity of the plasma membrane occurs during axonotmesis, and this discontinuity prevents the propagation of action potentials. Surrounding the nerve cell is a high extracellular calcium medium. When axons are damaged or severed, this extracellular calcium enters the peripheral nerve cell; this rush of calcium triggers the release of vesicles attached to the axonal microtubule system. These vesicles have a repair function and serve to seal the lipid bilayer, salvaging proximal axons and cell bodies. However, the distal axons undergo the Wallerian degeneration degradation process, resulting in distal axonal stump breakdown over the following week. This is why irrigation with a calcium-free solution is a critical component in PEG fusion—it prevents vesicle release and premature axonal stump fusion before cut axonal ends are mechanically reapproximated7. The addition of calcium-free solutions such as methylene blue cause the axon ends to remain patent, and the added PEG, hydrophilic in nature, helps remove water from the damaged lipid bilayer of the plasmalemma. This lowers the activation energy for plasmalemma fusion. Any remaining apertures are sealed with a calcium-containing solution, which causes any vessels not previously activated to interact with the plasmalemma, sealing it from ionic transition6.
While several studies have confirmed the usefulness of PEG in treating peripheral nerve injuries, the comparative advantages and disadvantages of PEG compared to other therapeutic treatments have not been definitively shown in the literature. The overall goal of this systematic review is to provide a comprehensive evaluation of existing literature concerning the outcomes of PEG treatment on peripheral nerve regeneration in preclinical models.
Methods
A systematic review of literature was performed on articles published about preclinical studies involving PEG treatment of peripheral nerve injury. Data extraction was conducted on the results of articles meeting this review’s inclusion criteria. Once the data was extracted, extensive analysis of the data was completed.
Search methods
The literature review was conducted under the guidelines of Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA, Figure 1). The MEDLINE database was queried using PubMed using the following keywords and phrases: “polyethylene glycol” OR “PEG” AND “nerve” AND “fusion”.
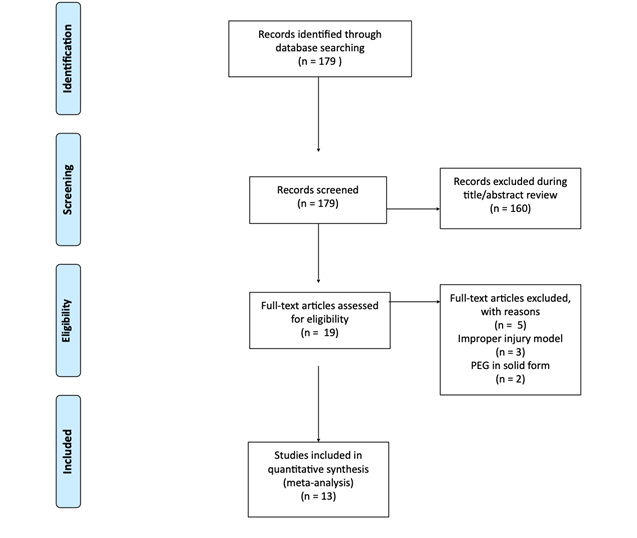
Figure 1: PRISMA Flow Diagram of the Literature Search.
Selection criteria
The inclusion criteria included articles that reported in vivo PEG treatment in animal models. After all of the articles were compiled, duplicate titles were removed. The two authors of this study, D.B.R. and S.C.C., then analyzed the remaining titles and abstracts. All included preclinical studies contained the treatment of a group with PEG after a peripheral nerve injury. Articles that published in a language other than English were excluded, as were any studies involving human research. Conference presentations and videos were not included in the criteria. Efforts were first made to determine the relevancy of the article from the abstract; if this could not be achieved, the full text was analyzed.
Data collection and analysis
Data extraction was performed by D.B.R. and S.C.C. during the spring of 2021. The following data measures were collected from the studies that met inclusion criteria: nerve type, lesion type, methods of evaluation, and outcomes. Nerve type referred to the specific peripheral nerve being treated; outcomes included morphological, functional, and electrophysiological. The advantages of using PEG as a treatment for peripheral nerve injury were compared to controls, and then the amount of significant findings in each of the data measures was evaluated.
Results
During the initial search of the literature, one hundred and seventy-nine articles were identified. After the application of inclusion and exclusion criteria, thirteen on animal models were identified. Only one of the studies utilized guinea pigs as the model, while the rest utilized rats. Ten examined the sciatic nerve, two involved the facial nerve, and one the femoral nerve. Distinctions were made for studies that evaluated peripheral nerve crush injuries versus cut injuries.
The results of the preclinical studies examined were evaluated through three different types of tests and/or recordings: motor, electrophysiological, and histological. The motor function was evaluated through the Sciatic Functional Index, or SFI. The SFI is a widely used metric in the study of the pathology of peripheral nerve injury. It is determined by comparing the geometric representation of the affected hind paw to the contralateral paw. Both are dipped in ink and the length and width of the print left by the rat as it walks across a piece of paper are measured7. In the nine of the thirteen studies that recorded this measure all except one reported an improve outcome8. This is likely most clinically relevant recording of the three so the fact that SFI improved after PEG treatment is indicative of its usefulness in PNI treatment.
Electrophysiological parameters were also measured in eleven of the thirteen studies. These measures included compound muscle action potential (CMAP) and force of muscle contraction. The restoration of compound muscle action potentials to normal levels and in turn force of muscle contraction is an indicator that PEG-mediated axonal fusion has been a success; the majority of studies reviewed showed that CMAP’s were restored to normal levels.
Histological examinations are likely the most objective of the three categories of data analyzed. There were two main relevant histological outcomes encountered in the literature: number of axons in sites distal to the location of the peripheral nerve injury and the diameter of these axons. In the majority of studies, either one or both of these was reported to be improved9-12.
Of the thirteen preclinical studies analyzed, only Brown et. al14 did not record PEG treatment having any sort of preferential outcomes compared to the control group. It is worth noting that this is one of only two studies that examined the facial nerve14. There are several possible explanations for this. This study conducted histological analysis on muscle rather than nerve and came to the conclusion that PEG treatment must not be useful for the facial nerve. However, analysis of their results and conclusion indicate that the study makes several assumptions; Bittner et al17 concludes that the lack of peripheral nerve fusion in the study by Brown et al14. is likely due to the incorrect use of solutions18.
Two final clinically significant findings involved the actual process of applying the PEG treatment to the peripheral nerve. The first of these that should be noted is that methylene blue is the only solution that was shown to significantly enhance nerve fusion when applied before PEG treatment15. Other substances, such as methylprednisolone, melatonin, protein kinase C isozyme η pseudosubstrate fragment (ηPSF), and protein kinase A inhibitor (PKI), were almost completely unsuccessful22-25. In addition, Riley et. al16 examined the use of a device that increases the consistency of PEG application. This device improved electrophysiological CMAP recovery by 12%.
Discussion
PEG therapy in the treatment of peripheral nerve injuries questions the idea that axon severance leads to the irreversible degeneration of the distal axon. The results of the preclinical studies examined in this systematic review of the literature show the future of PEG nerve fusion in clinical practice to be promising. However, there are still some areas to be reviewed. Almost all of the studies included measures of motor function recovery, but few examined any sort of metric for sensory recovery. Preclinical studies that review sensory recovery of the dermatomes covered by the damaged peripheral nerves would be helpful in establishing PEG treatment. Also, a more thorough investigation of autonomic nerve function after PEG treatment should be conducted, as the literature in this area is also lacking.
The effect of PEG on peripheral myelination, particularly Schwann cells, should also be investigated; none of these studies indicated whether PEG treatment of nerve injury prevents Schwann cell death. An animal study or series of animal studies that measured the post-treatment rate of survival of damaged Schwann cells would clarify this. Establishing a timeline for when PEG treatment is too late to be used clinically would also help set some guidelines. Bamba et al13 reported successful fusion of a rat sciatic nerve twenty-four hours after nerve injury, which could be used as a benchmark upon which to further analyze the maximal feasible time gap in injury-to-intervention. Despite these mildly uncertain aspects, this systematic review shows the future of PEG nerve fusion as a viable clinical treatment of peripheral nerve injuries is bright.
Table 1:Summary of Study Characteristics
|
Investigator, Year |
Animal Model |
Nerve Type |
Injury Type(s) |
Behavioral analysis |
Histological Analysis |
Electrophysiological Analysis |
PEG Repair Superiority Recorded |
PEG % and Composition |
|
Bittner et. al, 2012 24 |
Rat |
Sciatic |
Crush, Cut |
Y |
N |
Y |
Y |
50%, (-) |
|
Mikesh et. al, 2018 15 |
Rat |
Sciatic |
Cut |
Y |
Y |
Y |
Y |
50%, 3.35 kDa |
|
Stavisky et. al, 2005 25 |
Rat |
Sciatic |
Crush |
N |
N |
Y |
Y |
50%, (-) |
|
Brown et. al, 2018 18 |
Rat |
Facial |
Cut |
Y |
Y |
N |
N |
50%, 3.35 kDa |
|
Isaacs et. al, 2009 26 |
Rat |
Sciatic |
Cut |
N |
Y |
Y |
Y |
(-), (-) |
|
Ghergherehchi et. al, 2018 29 |
Rat |
Sciatic |
Crush, Cut |
Y |
Y |
Y |
Y |
50%, 3.30 kDa |
|
Mikesh et. al, 2018 14 |
Rat |
Sciatic |
Cut |
Y |
Y |
Y |
Y |
50%, 3.35 kDa |
|
Britt et. al, 2010 8 |
Rat |
Sciatic |
Crush, Cut |
Y |
N |
Y |
Y |
50%, 2 kDa |
|
Salomone et. al, 2018 13 |
Rat |
Facial |
Cut |
N |
Y |
Y |
Y |
50%, (-) |
|
Sexton et. al, 2012 28 |
Rat |
Sciatic |
Cut |
Y |
Y |
Y |
Y |
50%, (-) |
|
Riley et. al, 2015 32 |
Rat |
Sciatic |
Cut |
Y |
Y |
Y |
Y |
50%, 2 kDa |
|
Robinson et. al, 2016 30 |
Rat |
Femoral |
Cut |
N |
Y |
N |
N |
50%, (-) |
|
Donaldson et. al, 2002 31 |
Guinea Pig |
Sciatic |
Crush |
N |
N |
Y |
Y |
50%, 3.35 kDa |
Given the great success in animal models and low risk profile of the PEG substances, investigators have advocated for an early transition of PEG fusogen to human investigations15. To our knowledge Bamba et al13. were the first to successfully utilize PEG technology in human digital nerve injuries. The patients who received PEG had superior clinical outcomes and faster sensory recovery compared to a group of control patients with similar injuries21. We initiated a pilot study to evaluate the preliminary findings of PEG therapy in human upper extremities traumatic nerve injuries as well as identify any adverse events. Here we report our early repair findings in nerve recovery found in the first four patients enrolled. In this ongoing randomized control trial, we used PEG treatment for human peripheral nerve repair. The nerves repaired included two radial digital nerves, one median nerve, and one ulnar nerve. Results demonstrated meaningful or complete recovery in three of the four subjects25 (Fig. 2). Additionally, an ulnar nerve repair at the wrist, and a radial digital nerve repair with an autograft, experienced meaningful recovery within four weeks, which is much earlier than typical expectations for recovery. This data demonstrates a proof of concept of PEG 3350KD can be used in human trials with no adverse responses.
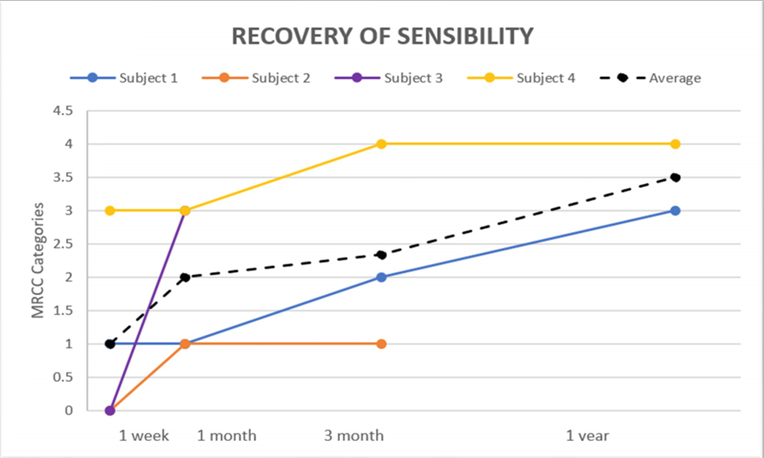
Figure 2: Recovery of sensibility in damaged nerves using a PEG fusion. A Medical Research Council Classification (MRCC) of S0 corresponds to a numerical value of 0, S1-S2 corresponds to 1, S3 to 2, S3+ to 3, and S4 to 4. A MRCC of S3, or 2, is denoted as meaningful clinical recovery.
Based on this systematic review and despite this limited case series, the use of PEG solution for PNI treatment is very promising with significant implications in humans. Future randomized clinical studies are needed to consolidate our findings.
References
- Grinsell D, Keating CP. Peripheral nerve reconstruction after injury: a review of clinical and experimental therapies. Biomed Res Int. 2014; 2014:698256. doi: 10.1155/2014/698256. Epub 2014 Sep 3. PMID: 25276813; PMCID: PMC4167952.
- Beris A, Gkiatas I, Gelalis I, et al. Current concepts in peripheral nerve surgery. Eur J Orthop Surg Traumatol. 2019 Feb; 29(2):263-269. doi: 10.1007/s00590-018-2344-2. Epub 2018 Nov 27. PMID: 30483968.
- Henderson PW. Immediate and complete restoration of peripheral nerve function after injury is attainable by a combination of surgical and chemical interventions. Med Hypotheses. 2018; 113:65-67.
- Bailey FE, Koleske JV. Alkylene oxides and their polymers. New York: Dekker. 1990; 27–28. ISBN 9780824783846. Retrieved 17 July 2017.
- Yoo S, Nguyen MP, Fukuda M, et al. Plasmalemmal sealing of transected mammalian neurites is a gradual process mediated by Ca(2+)-regulated proteins. J Neurosci Res. 2003; 74(4):541-551.
- Britt JM, Kane JR, Spaeth CS, et al. Polyethylene Glycol Rapidly Restores Axonal Integrity and Improves the Rate of Motor Behavior Recovery After Sciatic Nerve Crush Injury. J Neurophysiol. 2010 Aug;104(2):695-703. doi: 10.1152/jn.01051.2009. Epub 2010 May 5.
- Monte-Raso VV, Barbieri CH, Mazzer N, et al. Is the Sciatic Functional Index always reliable and reproducible? J Neurosci Methods. 2008 May 30; 170(2):255-61. doi: 10.1016/j.jneumeth.2008.01.022. Epub 2008 Feb 2. PMID: 18325595.
- Sexton KW, Rodriguez-Feo CL, Boyer RB, et al. Axonal fusion via conduit-based delivery of hydrophilic polymers. Hand (N Y). 2015; 10: 688–
- Riley DC, Bittner GD, Mikesh M, et al. Polyethylene glycol-fused allografts produce rapid behavioral recovery after ablation of sciatic nerve segments. Neurosci. Res. 2015; 93(4): 572–583.
- Salomone R, Jacomo AL, Nascimento SBD, et al. Polyethylene glycol fusion associated with antioxidants: A new promise in the treatment of traumatic facial paralysis. Head Neck. 2018; 40: 1489–
- Mikesh M, Ghergherehchi CL, Hastings RL, et al. Polyethylene glycol solutions rapidly restore and maintain axonal continuity, neuromuscular structures, and behaviors lost after sciatic nerve transections in female rats. Neurosci. Res. 2018; 96, 1223–1242.
- Mikesh M, Ghergherehchi CL, Rahesh S, et al. Polyethylene glycol treated allografts not tissue matched nor immunosuppressed rapidly repair sciatic nerve gaps, maintain neuromuscular functions, and restore voluntary behaviors in female rats. Neurosci. Res. 2018; 96: 1243–1264.
- Bamba R, Riley DC, Kim JS, et al. Evaluation of a Nerve Fusion Technique with Polyethylene Glycol in a Delayed Setting After Nerve Injury. Hand Surg. 2018; 43: 82e81–82e87.
- Brown BL, Asante T, Welch HR, et al. Functional and Anatomical Outcomes of Facial Nerve Injury with Application of Polyethylene Glycol in a Rat Model. JAMA Facial Plast. Surg. 2018.
- Ghergherehchi CL, Shores JT, Alderete J, et al. Methylene blue enhances polyethylene glycol-fusion repair of completely severed rat sciatic nerves. Neural Regen Res. 2021 Oct;16(10):2056-2063. doi: 10.4103/1673-5374.308099. PMID: 33642394.
- Riley DC, Boyer RB, Deister CA, et al. Immediate Enhancement of Nerve Function Using a Novel Axonal Fusion Device After Neurotmesis. Ann Plast Surg. 2017 Dec;79(6):590-599. doi: 10.1097/SAP.0000000000001242.
- Bittner GD, Ghergherehchi CL, Mikesh M. Surgical Technique and Other Protocols Used Probably Did Not Induce Polyethylene Glycol Fusion of Rat Facial Nerves. JAMA Facial Plast Surg. 2019 Jan 1;21(1):81. doi: 10.1001/jamafacial.2018.1126.
- Bittner GD, Keating CP, Kane JR, et al. Rapid, effective, and long-lasting behavioral recovery produced by microsutures, methylene blue, and polyethylene glycol after completely cutting rat sciatic nerves. J. Neurosci Res. 2012; 90: 967–980.
- Stavisky RC, Britt JM, Zuzek A, et al. Melatonin enhances thein vitroandin vivorepair of severed rat sciatic axons. Neurosci. Lett. 2005; 376, 98–101.
- Isaacs J, Klumb I, McDaniel C. Preliminary investigation of a polyethylene glycol hydrogel “nerve glue” J Brachial Plex Peripher. Nerve Inj. 2009; 4: 16.
- Sexton KW, Pollins AC, Cardwell NL, et al. Hydrophilic polymers enhance early functional outcomes after nerve autografting. J. Surg. Res. 2012; 177: 392–400
- Ghergherehchi CL, Bittner GD, Hastings RL, et al. Effects of extracellular calcium and surgical techniques on restoration of axonal continuity by polyethylene glycol fusion following complete cut or crush severance of rat sciatic nerves.J Neurosci Res. 2016 Mar;94(3):231-45. doi: 10.1002/jnr.23704. Epub 2016 Jan 5.
- Robinson GA, Madison RD. Polyethylene glycol fusion repair prevents reinnervation accuracy in ratperipheral nerve. J Neurosci Res. 2016; 94: 636–644.
- Donaldson J, Shi R, Borgens R. Polyethylene glycol rapidly restores physiological functions in damaged sciatic nerves of guinea pigs. 2002 Jan; 50(1):147-56; discussion 156-7. doi: 10.1097/00006123-200201000-00023.
- Glassman GE, Black J, Pollins A, et al. Preliminary Outcomes from a Randomized Control Trial using Adjunct Polyethylene Glycol Therapy for Human Peripheral Nerve Repair; Abstract presented at: American Association for Hand Surgery. January 2021.
